Archive for June, 2012
MAMMOGRAPHY & BREAST IMPLANTS
Submitted on June 25, 2012
The purpose of a mammogram is to identify abnormalities or changes in breast tissue. Screening mammograms can detect these abnormalities at an early stage resulting in potenti...
Read More >>BODY CONTOURING AFTER WEIGHT LOSS SURGERY
Submitted on June 20, 2012
After weight loss surgery, resuming normal life can be a challenge. The most significant change is the amount of food that can be eaten. Most weight loss surgeries reduce stom...
Read More >>
Daxxify: A New Long-Lasting Alternative to BOTOX® Cosmetic
In the ever-changing world of cosmetics, one thing has remained constant: BOTOX® Cosme...
Facial Aging
Eyelids
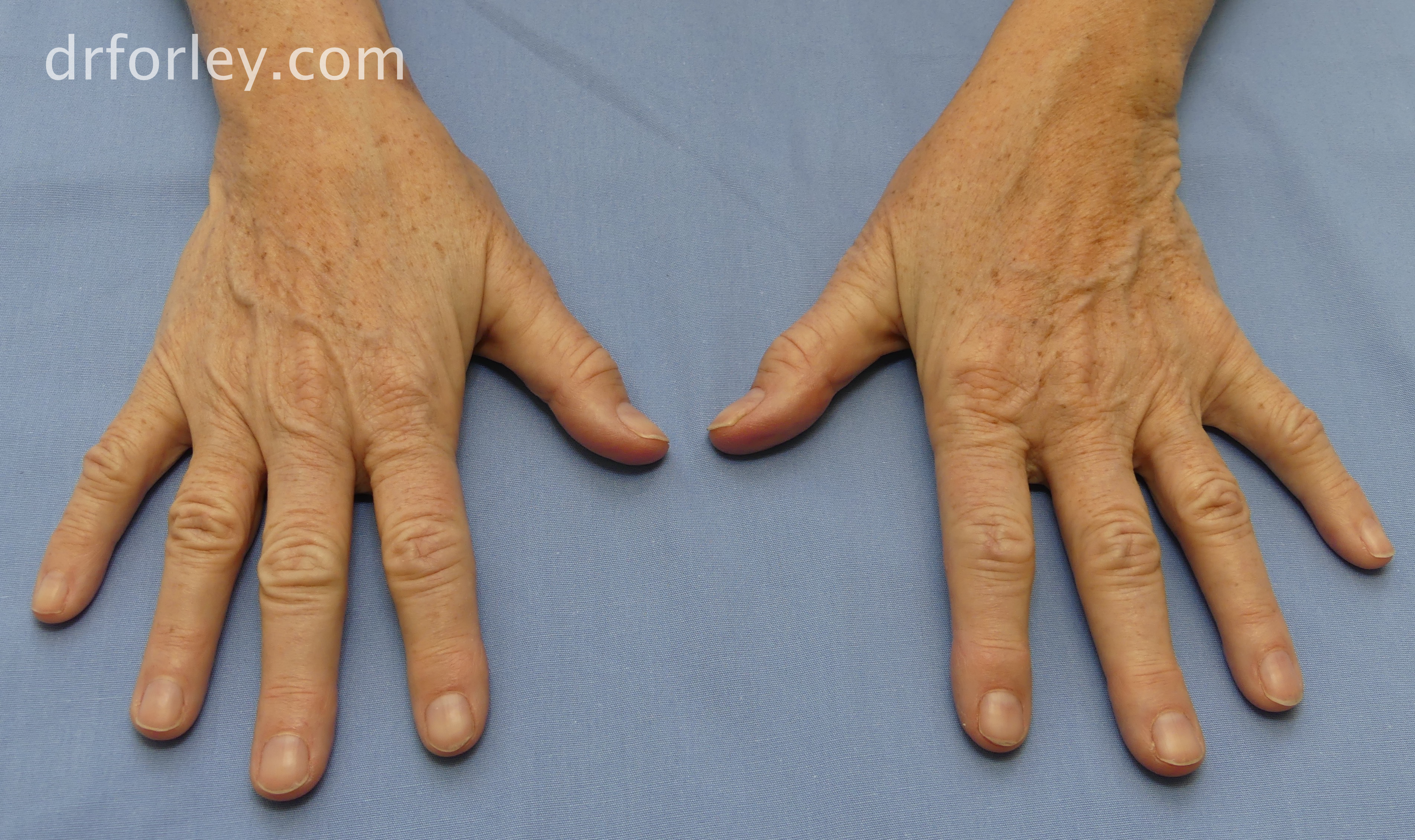
Hands
Body Contouring
Breast Augmentation
Breast Reduction
Brow Lift
Energy Devices
Eyelid Surgery
Facelift
Gynecomastia
Injectable Fillers
Liposuction
Men Surgical
Necklift
Neuromodulators
Non-Surgical
Lasers
Nose Surgery
Nutrition
Plastic Surgery
Plastic Surgery Advice
Skin Care
Skin Tightening
Skin Tightening test
Tummy Tuck
Uncategorized